
Choose a channel
Check out the different Progress in Mind content channels.

Progress in Mind

The Value of Treatment (VoT) Project is a timely and ground-breaking initiative of the European Brain Council (EBC). It argues that optimizing interventions in mental health and neurological diseases can bring both positive outcomes for patients and socio-economic gains for society. The Project aims to support its views with robust empirical data, and to make policy recommendations from solid scientific knowledge.
Based on two years of research, the Project identifies current problems along the entire care pathway, from prevention through screening, diagnosis and treatment, to follow-up and rehabilitation – and then proposes solutions. Early detection and prompt intervention are regarded as the starting point, with greater use of evidence-based guidelines for screening.
Fundamental to treatment is the planning of coordinated, multidisciplinary, patient-centered care. Along with this goes patient education and empowerment to encourage adherence and compliance. Electronic reminder systems exemplify the potential value of e-health tools.
General policy recommendations made by the EBC are: the need to assess the impact of brain diseases on the outcome of other medical conditions; health systems evaluation so that effective interventions can be identified and then replicated in similar settings; the establishment of common research platforms (Knowledge Hubs) to share data; and the encouragement of EU-wide initiatives in brain health to promote collaboration.
Health is wealth: In Europe, the direct and indirect costs of brain disorders exceed 800 billion euros each year – more than CVD, cancer and diabetes combined
The EBC recognizes the burden suffered by affected individuals, their families, friends and carers – but also by society at large. In Europe, the annual direct and indirect costs of brain disorders exceed 800 billion Euros1 – more than cardiovascular disease (CVD), cancer and diabetes combined. Yet our total research expenditure on brain disorders is smaller than the expenditure on each of these disease areas.
As we deal more effectively with CVD and even with cancer, brain diseases come to the fore. Society has not yet caught up with this fact, but Professor David Nutt, chair of the EBC, along with the other members of the Council, are determined that it should.
Greater clinical benefit for patients with brain disorders and gains in cost-effectiveness for society -- both can be achieved by earlier intervention, closer co-ordination of multidisciplinary car
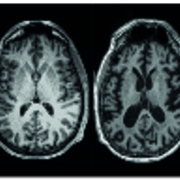

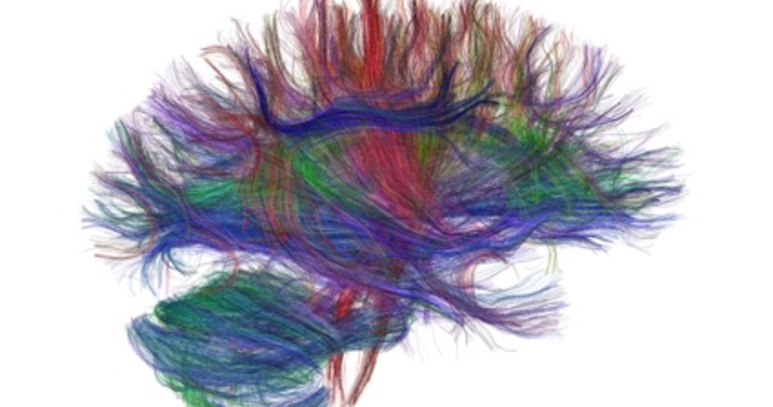
Brain imaging has advanced massively in the past two decades. Modern tools such as positron emission tomography (PET), magnetic resonance imaging (MRI) and Magnetoencephalography (MEG) allow us a much clearer view of how the brain works: we can almost literally “look inside the skull” (Camprodon & Stern, 2013). This article introduces the different forms of imaging and give examples of how we can use them to ask important questions in psychiatry and neurology.
We can consider imaging techniques from several perspectives. One is based on the detection instruments or technology used. Another is the kinds of signal that can be detected whether structural or functional or metabolic and yet another approach is to explore what they can be used for.

Brain imaging has advanced massively in the past two decades. Modern tools such as positron emission tomography (PET), magnetic resonance imaging (MRI) and Magnetoencephalography (MEG) allow us a much clearer view of how the brain works: we can almost literally “look inside the skull”. This article introduces the different forms of imaging and give examples of how we can use them to ask important questions in psychiatry and neurology.
We can consider imaging techniques from several perspectives. One is based on the detection instruments or technology used. Another is the kinds of signal that can be detected whether structural or functional or metabolic and yet another approach is to explore what they can be used for.

Brain imaging has advanced massively in the past two decades. Modern tools such as positron emission tomography (PET), magnetic resonance imaging (MRI) and Magnetoencephalography (MEG) allow us a much clearer view of how the brain works: we can almost literally “look inside the skull”. This article introduces the different forms of imaging and give examples of how we can use them to ask important questions in psychiatry and neurology.
We can consider imaging techniques from several perspectives. One is based on the detection instruments or technology used. Another is the kinds of signal that can be detected whether structural or functional or metabolic and yet another approach is to explore what they can be used for.

Brain imaging has advanced massively in the past two decades. Modern tools such as positron emission tomography (PET), magnetic resonance imaging (MRI) and Magnetoencephalography (MEG) allow us a much clearer view of how the brain works: we can almost literally “look inside the skull”. This article introduces the different forms of imaging and give examples of how we can use them to ask important questions in psychiatry and neurology.
We can consider imaging techniques from several perspectives. One is based on the detection instruments or technology used. Another is the kinds of signal that can be detected whether structural or functional or metabolic and yet another approach is to explore what they can be used for.



The burden of brain disease in Europe continues to rise. Currently, more than one in three individuals in Europe suffers from a disorder of the brain.1 Brain diseases carry with them an estimated yearly economic burden of 789 billion Euro,2 placing a considerable burden on personal, social, and economic well-being. Globally, mental disorders account for a disproportionately large percentage of disability-adjusted life years (56.7%) followed by neurological disorders (28.6%),3 illustrating the deleterious effects these disorders place on the individual and society. Efforts to reduce this burden have led to a multi-disciplinary collaboration between the neurosciences, sociologists, clinicians, and public health officials, with a particular focus on the interplay between genetics and the environment, often referred to as “nature versus nurture”, in the development of these diseases.
Gaining a better understanding of the causal risk factors associated with psychiatric and neurological disease may aid in efforts to prevent the development of these often disabling conditions and subsequently reduce this burden overall.
Dr. Andreas Meyer-Lindenberg addresses the need and potential approach one could undertake to better understand and potentially prevent the development of these disorders